ENFERMEDAD CENICIENTA O ERITEMA DISCRÓMICO PERSTANS, ACTUALIZACIÓN
En el año de 1.957 Oswaldo Ramírez en el primer Congreso Centro Americano de Dermatología describió por vez primera una dermatosis encontrada en su País, EL SALVADOR, con el nombre de "LOS CENICIENTOS, PROBLEMA CLÍNICO".
En 1.961 Convit y Colaboradores consideraron esta enfermedad una variante del ERITEMA PERSTANS y la denominaron ERITEMA CRÓNICO FIGURADO con MELANODERMIA.
SÍNTOMAS CLÍNICOS:
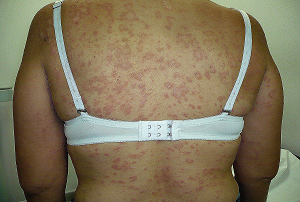
El ERITEMA DISCRÓMICO PERSTANS, se manifiesta principalmente en adultos jóvenes, y esta caracterizado por la aparición de manchas o máculas de color gris o "ceniza", (ENFERMEDAD CENICIENTA), las cuales se presentan principalmente en tórax anterior, cara , cuello y brazos, pero puede presentarse también en abdomen y piernas, incluso la membrana mucosa de la boca, sin ninguna otra sintomatología orgánica; no pican, ni molestan. En casos poco frecuentes ha sido descrita en niños.
ETIOLOGÍA:
Se dice, se especula, que la enfermedad es producida por el contacto de FERTILIZANTES utilizados en la agricultura e industria, los cuales contienen un químico denominado NITRATO de AMONIO, también ha sido relacionada con CONTRASTES RADIOLÓGICOs, PARASITOSIS, MEDICAMENTOS, y los ANTÍGENOS DE HISTOCOMPATIBILIDAD (HLA DR4), más actualmente sigue considerándose que la causa es DESCONOCIDA.
El hecho de que esta patología ha sido observada en muchos trabajadores del campo (agricultores) es lo que hizo relacionarla con el NITRATO DE AMONIO, componente químico de los FERTILIZANTES.
TRATAMIENTO:
No existe tratamiento especifico para esta patología.se ha utilizado la CLOFAZIMINA o LAMPREN, la cual es utilizada en el tratamiento de la Lepra, porque induce hiperpigmentación de la piel y ayuda a disimular las manchas, otros elementos usados son la fotoprotección y la utilización de "fórmulas magistrales" tipo "BLANQUEADORES" para aclarar el color grisáceo de las lesiones.
La enfermedad fue aceptada como una nueva entidad nosológica en el 5to. Congreso Ibero Latino Americano de Dermatología Celebrado en Buenos Aires, ARGENTINA en el año 1963, con el nombre de ERITEMA DISCRÓMICO PERSTANS.
En Al año de 1.967 el mismo Oswaldo Ramírez describe un estudio epidemiológico de 139 casos bajo el nombre de DERMATOSIS CENICIENTA, o ERITEMA DISCRÓMICO PERSTANS (EDP). Después de esta primera descripción comenzaron a reportarse numerosos casos en MUCHOS PAÍSES.
En la Década de los 80 algunos autores comienzan a especular la posibilidad de que el ERITEMA DISCRÓMICO PERSTANS, es una variante del LIQUEN PLANO. Algunos lo denominaron LIQUEN PLANO PIGMENTOSO, esto en base a las siguientes características:
SIMILITUDES:
1. El LIQUEN PLANO y el ERITEMA DISCRÓMICO PERSTANS tienen UN MISMO PATRÓN histopatológico: Una Dermatitis Liquenoide.
2.) El liquen plano se presenta a veces como manchas grisáceas y también se presenta en personas que manipulan CONTRASTES RADIOLÓGICOS.
3.) Se describieron casos de localización clínica con patrón ZOSTERIFORME en ambas..
4.) Se han descrito casos de ERITEMA DISCRÓMICO PERSTANS asociados a medicamentos. Esto también ha sido descrito en el LIQUEN PLANO.
5.) El tratamiento es bastante difícil en ambos.
En 1984. Ramírez de nuevo hace una revisión sobre todos los casos publicados y concluye que NO ES UNA ENFERMEDAD TROPICAL, sino de distribución mundial, más NO LA ASOCIA con LIQUEN PLANO.
42 años después la controversia continua e incluso algunos autores hablan de 2 variantes de ERITEMA DISCRÓMICO PERSTANS, Otros continúan insistiendo en que debería unificarse el criterio de esta forma:
ERITEMA DISCRÓMICO PERSTANS, como una variante de LIQUEN PLANO, bajo la sinonimia de LIQUEN PLANO PIGMENTOSO. Yo estoy de acuerdo con esto 100% , pero creo que debe respetarse el NOMBRE ORIGINAL.
NOTA: Para hoy día año 2025 esta patología es reconocida MUNDIALMENTE con el nombre de ERITEMA DISCRÓMICO PERSTANS, o ENFERMEDAD "CENICIENTA", como fue propuesto en el año 1963, y su descubridor OSWALDO RAMÍREZ del SALVADOR, Sur América.
Saludos a todos !!!
Dr. José Lapenta R.,,,
EDITORIAL ENGLISH:
In 1957 Oswaldo Ramírez, during the First Central-American Dermatology Congress in El Salvador; described for the first time a dermatosis found in his country, EL SALVADOR, with the name "THE ASHY,CLINICAL PROBLEM".
In 1961, Convit et al. consider this disease as a variant of ERYTHEMA PERSTANS and named it "CHRONIC FIGURED ERYTHEMA with MELANODERMA".
CLINICAL SYMPTOMS:
ERYTHEMA DYSCHROMICUM PERSTANS primarily occurs in young adults and is characterized by the appearance of gray or "ashy" spots or macules (ASHY DISEASE). These spots appear primarily on the anterior chest, face, neck, and arms, but can also appear on the abdomen and legs, even the mucous membrane of the mouth, without any other organic symptoms; they are not itchy or bothersome. In rare cases it has been described in children.
ETIOLOGY:
It is said and speculated that the disease is caused by contact with FERTILIZERS used in agriculture and industry, which contain a chemical called AMMONIUM NITRATE. It has also been linked to RADIOLOGICAL CONTRAST AGENTS, PARASITES, DRUGS and HISTOCOMPATIBILITY ANTIGENS (HLA DR4), However, the cause is currently still considered unknown.
The fact that this condition has been observed in many farm workers (FARMERS) is what led to its association with AMMONIUM NITRATE, a chemical component of fertilizers.
TREATMENT:
There is no specific treatment for this condition. CLOFAZIMINE or LAMPREN has been used in the treatment of leprosy because it induces skin hyperpigmentation and helps conceal the color of the spots. Other elements used include SUNSCREENS and the use of "magistral formulas" such as "BLEACHING AGENTS" to lighten the grayish color of the lesions.
This disease was accepted as new nosologic entity in the Fifth Congress of the Ibero-Latin-American College of Dermatology in Buenos Aires, ARGENTINE in the year 1963 with the name of "ERYTHEMA DYSCHROMICUM PERSTANS" (EDP).
In To the year of 1.967 the same Oswaldo Ramirez describes an epidemiologic study of 139 cases under the name of ASHY DERMATOSIS or ERYTHEMA DYSCHROMICUM PERSTANS. After this first description they began to be reported numerous cases in MANY COUNTRIES.
In the decade of the 80 some authors begin to speculate the probability that the ERYTHEMA DYSCHROMICUM PERSTANS is a variant of THE LICHEN PLANUS. Some denominated it LICHEN PLANUS PIGMENTOSUS, this based on the following ones characteristic:
SIMILARITIES:
1. The LICHEN PLANUS and THE ERYTHEMA DYSCHROMICUM PERSTANS have the same histopathological picture: A Lichenoid Dermatitis.
2.) The lichen planus is sometimes presented as ashy macules, and also occurs in people who handle RADIOLOGICAL CONTRASTS.
3.) Cases of clinical localization were described with ZOSTERIFORM pattern in both.
4.) Cases of ERYTHEMA DYSCHROMICUM PERSTANS associated to medications have been described. This has also been described in association with LICHEN PLANUS.
5.) The treatment is quite difficult in both.
In 1984. Ramirez again makes a revision on all the published cases and it concludes that it IS NOT A TROPICAL ILLNESS, but of world-wide distribution, but IT DOESN'T associate it with LICHEN PLANUS.
42 years later the controversy continuous and some authors even speak of 2 variants of ERYTHEMA DYSCHROMICUM PERSTANS, Others continue insisting in that it should become unified the approach in this way:
ERYTHEMA DYSCHROMICUM PERSTANS, a variant of LICHEN PLANUS, under the synonymy of LICHEN PLANUS PIGMENTOSUS. I agree with this in 100%.but I think it should keep its ORIGINAL NAME
NOTE: For today, in the year 2025, this pathology is recognized WORLDWIDE with the name ERYTHEMA DYSCROMICUM PERSTANS or ASHY DERMATOSIS, as it was proposed in 1963, and its discoverer OSWALDO RAMÍREZ from SALVADOR, South America.
Greetings to all!!!
Dr. José Lapenta R.,,,
===============================================================
REFERENCIAS BIBLIOGRÁFICAS / BIBLIOGRAPHICAL REFERENCES
================================================================
================================================================
B.- Ashy dermatosis: a review (2019).
C.- Ashy dermatosis with involvement of mucous membranes (2017).
D. - Skin Weathering and Ashiness in Black Africans (2003).
E. Rare ashy dermatosis-like hyperpigmentation associated with osimertinib (2022).
F.- A retrospective clinico-pathological study comparing lichen planus pigmentosus with ashy dermatosis (2018).G.- Ashy Dermatosis and Lichen Planus Pigmentosus: The Histopathological Differences (2019).
================================================================
1.) "Los cenicientos. Problema Clinico". (The Ashy. Clinical problem)
2.) "Eritema Discromico Perstans" (Eritema figurado cronico con melanodermia).(Chronic Figured Erythema with Melanodermia)
3.) Sobre la Etiopatogenia del eritema discrómico perstans (Dermatosis Cenicienta). Posibilidad de una Melanosis Neuro-cutánea
4.) The ashy dermatosis (erythema dyschromicum perstans)
5.) Ashy dermatosis or lichen planus pigmentosus: what is in a name?
6.) ERYTHEMA DYSCHROMICUM PERSTANS (ASHY DERMATOSIS) THE ENTITY
7.) [Ashy dermatitis. Comments on 2 clinical forms].
8.) Unilateral ashy dermatosis occurring in a child.
9.) [Current status of ashy dermatosis. Synonym--erythema dyschromicum perstans].
10.) [Ashy-dermatosis--a case with spontaneous disappearance of the cutaneous lesions].
11.) Erythema dyschromicum perstans and lichen planus.
12.) Ashy dermatosis. An apoptotic disease?
13.) Ashy dermatosis--a variant of lichen planus?
14.) Erythema dyschromicum perstans in early childhood.
15.) Fixed drug eruption presenting as erythema dyschromicum perstans: a flare without taking any medications.
16.) Reticulate postinflammatory hyperpigmentation with band-like mucin deposition.
17.) Erythema dyschromicum perstans: report of a new case and critical review of the literature.
18.) Involvement of cell adhesion and activation molecules in the pathogenesis of erythema dyschromicum perstans (ashy dermatitis). The effect of clofazimine therapy.
19.) Periorbital hyperpigmentation and erythema dyschromicum perstans.
20.) Erythema dyschromicum perstans and lichen planus: are they related?
21.) Erythema dyschromicum perstans. Immunopathologic studies.
22.) Simultaneously active lesions of vitiligo and erythema dyschromicum perstans.
23.) Mononuclear cell subpopulations and infiltrating lymphocytes in erythema dyschromicum perstans and vitiligo.
24.) Chlorothalonil, a possible cause of erythema dyschromicum perstans (ashy dermatitis).
25.) Lichen planus pigmentosus presenting in zosteriform pattern.
26.) [Erythema dyschromicum perstans versus lichen planus].
27.) Erythema dyschromicum perstans.
28.) Erythema dyschromicum perstans.
29.) [Erythema cinitiensis perstans].
30.) [Idiopathic eruptive macular pigmentation].
31.) [Erythema dyschromicum perstans].
32.) Erythema dyschromicum perstans. A follow-up study from northern Finand.
33.) Ingestion of ammonium nitrate as a possible cause of erythema dyschromicum perstans (ashy dermatosis).
34.) [Erythema dischromicum perstans (ashy dermatosis). Report of two cases]. Pathologica 1993 Sep-Oct;85(1099):533-41
35.) [Ashy dermatosis].
36.) [Ashy dermatosis. Review of the literature and report of a case].
37.) [Ashy dermatosis (erithema dyschromicum perstans): prospective study of 23 patients].
38.) Reticulate, patchy and mottled pigmentation of the neck. Acquired forms.
39.) Lichen planus pigmentosus associated with acrokeratosis of Bazex.
40.) Ashy dermatosis and lichen planus pigmentosus: a clinicopathologic study of 31 cases.
41.) [Lichen ruber exanthematicus et pigmentosus in mercury poisoning. A contribution to individual pathology in occupational medicine].
42.) [Lichen planus and lichen planus pigmentosus following gold therapy--case reports and review of the literature].
43.) Lichen planus pigmentosus of the oral mucosa: a rare clinical variety.
================================================================ =====================================================================
1.) "Los cenicientos. Problema Clinico". (The Ashy. Clinical problem) Memoria del Primer Congreso Centro Americano de Dermatologia, San salvador,
1957:122-130 Ramirez, C.O
====================================================================
====================================================================
2.) "Eritema Discromico Perstans" (Eritema figurado cronico con melanodermia).(Chronic Figured Erythema with Melanodermia)
Dermat. Venezolana, 1961, 2:118-164
Convit, J., Kerdel-Vegas, F., Rodriguez, G.
====================================================================
3.) Sobre la Etiopatogenia del eritema discrómico perstans (Dermatosis Cenicienta). Posibilidad de una Melanosis Neuro-cutánea Derm Venez 1995;
33:149-151
Homez-Chacin, 1. Barroso T.
====================================================================
4.) The ashy dermatosis (erythema dyschromicum perstans): epidemiological study and report of 139 cases.
Ramirez C.O. Cutis 1967; 3:244-7
====================================================================
5.) Ashy dermatosis or lichen planus pigmentosus: what is in a name?
Arch Dermatol 1986 Feb;122(2):133
Bhutani LK
====================================================================
====================================================================
6.) ERYTHEMA DYSCHROMICUM PERSTANS (ASHY DERMATOSIS) THE ENTITY
====================================================================
SOURCE: Sobre la Etiopatogenia del eritema discrómico perstans (Dermatosis Cenicienta). Posibilidad de una Melanosis Neuro-cutánea
Derm Venez 1995;33:149-151 Homez-Chacin, 1. Barroso T.
ABSTRACT
In 1957 Oswaldo Ramírez, during the First Central-American DermatoIogy Congress in El Salvador; described for the first time a dermatosis found in his country wjth the name "The Ashy. Clinical problem". In 1961, Convit et al. consider this disease as a variant ot erythema perstans and name it "Chronic Figured Erythema with Melanodermia". this disease was accepted as new nosologic entity in the Fifth Congress of the Ibero-Latin-American College of Dermatology in Buenos Aires in 1963 with the name of "Erythema Dyschromicum Perstans".
According to O. Ramírez. "Erythema Discromicum Perstans (Ashy Dermatosis) is a chronic skin disease characterized by typical and marked changes in color of the skin (hyperpigmented macules, black-board gray, variable), of slow evolution, persistent, with no concomitant local alterations, but which sometimes have repercussions on the psychic state of the patient, according to the size of the lesion. It is not accompanied by any other cutaneous or symptomatic abnormality. It is not influenced by climate, racial, dietary or occupational factors". This dermatosis can appear at any age, from one to eighty years. Either sex can be equally affected, even though it is more frequent in females. lnitially lesions are localized, but they can become generalized, not involving scalp, annexes or palmo-plantar regions.
====================================================================
7.) [Ashy dermatitis. Comments on 2 clinical forms].
====================================================================
Med Cutan Ibero Lat Am 1986;14(2):95-9
Carvajal Huerta L, Uraga Pazmino E, Loayza Vivanzo E, Sabando Sanchez R, Garcia Atiaga I, Jeny E
The typical clinical characteristic of the ashy dermatitis is the fact that in case of light colored skin, the grey colour remains invariable. There is a new clinical form which is called the Brown Cinder Dermatitis which is characterized by a disciplined localization in the center of the face, trunk or upper extremities together with an inexorable change of the grey colour at the beginning to a brown colour at the end on the other it, has be enhanced the existence of the nummular form which is characterized by the existence of many greyish independent spots of circular or oval form mainly at the level of the trunk.
====================================================================
8.) Unilateral ashy dermatosis occurring in a child.
====================================================================
Arch Dermatol 1984 Nov;120(11):1491-3
Urano-Suehisa S, Tagami H, Iwatsuki K
An unusual case of ashy dermatosis of Ramirez occurred in a 5-year-old-girl who had ash-colored hyperpigmented macules and plaques on the left leg and the left side of the trunk. These unilateral lesions showed histopathologic changes of a lichenoid tissue reaction. Although the exact cause of ashy dermatosis remains unknown, the positive test result for serum rheumatoid factor and the granular deposition of IgM at the dermoepidermal junction found in our case has immunologic implications.
====================================================================
9.) [Current status of ashy dermatosis. Synonym--erythema dyschromicum perstans].
====================================================================
Med Cutan Ibero Lat Am 1984;12(1):11-8
[Article in Spanish]
Ramirez O, Lopez Lino DG
A clinical, histopathological, therapeutical and epidemiologic review of Ashy Dermatosis is done. This research has been taken from scientific publications, computers and personal communications. In twenty five years of scientific medical investigations it has not been determined its truth etiology , nor its therapeutic; this confirms it, as a new nosologic entity well defined.
The epidemiologic researches are concludent that this is not a tropical disease exclusively, but one of all over the world. We hope to obtain more references on this dermatosis throughout the Sessions of
Specialties of CILAD regarding this disease.
====================================================================
10.) [Ashy-dermatosis--a case with spontaneous disappearance of the cutaneous lesions].
====================================================================
Z Hautkr 1983 Jan 15;58(2):113-20
[Article in German]
Schneider I, Varga M, Zombai E, Husz S
A 14-years-old girl suddenly developed typical dermal signs of ashy-dermatosis at the time of menarche. After one year, the signs began to fade and had disappeared completely two years later. The direct immunofluorescence and the ultrastructure resemble lichen planus. Endocrine factors may have played a part in the presented case, considering the sudden onset at the time of menarche.
====================================================================
11.) Erythema dyschromicum perstans and lichen planus.
====================================================================
Arch Dermatol 1982 Sep;118(9):683-5
Naidorf KF, Cohen SR
Erythema dyschromicum perstans (EDP) is a cutaneous pigmentary disturbance originally considered to be a variant of erythema perstans. The nosologic identity of EDP has been challenged repeatedly as the number of patients with concurrent EDP-like eruptions and lichenoid disorders has increased. In this report, we describe a woman who had EDP for two years before the onset of classic lichen planus (LP).
The active lesions of LP gradually evolved into typical ashy-gray macules of EDP. This case provides further support for the concept that EDP and EDP-like conditions should be classified, in certain instances, as erythema dyschromicum variants of LP.
====================================================================
12.) Ashy dermatosis. An apoptotic disease?
====================================================================
Arch Dermatol 1981 Nov;117(11):701-4
Person JR, Rogers RS 3d
Of nine patients with ashy dermatosis, eight were women; most were young adults when the dermatosis began. The incidences of atopy (five patients) and thyroid disease (three patients) were striking.
Although some of the patients were clinically atypical, histologic study in all cases showed basal cell vacuolation, Civatte bodies, pigmentary incontinence, and a mild perivascular lymphohistiocytic infiltrate. Direct immunofluorescence microscopy, performed in four cases, showed igM cytoid bodies. We hypothesize that the postinflammatory hyperpigmentation in ashy dermatosis and, perhaps, in other dermatoses may occur on the basis of basal cell
apoptosis.
====================================================================
13.) Ashy dermatosis--a variant of lichen planus?
====================================================================
Cutis 1980 Jun;25(6):631-3
Kark EC, Litt JZ
Immunofluorescence studies on a patient with clinical and histological evidence of ashy dermatosis revealed a pattern commonly associated with lichen planus. In view of these findings, the possibility of a relationship between ashy dermatosis and lichen planus is suggested.
=================================================================
14.) Erythema dyschromicum perstans in early childhood. J Dermatol 1999 Feb;26(2):119-21
=================================================================
Lee SJ, Chung KY
Department of Dermatology, Yonsei University College of Medicine, Seoul, Korea.
Erythema dyschromicum perstans (EDP) is a rare disorder characterized by asymptomatic, slowly progressive, ash-gray macular pigmentation of the skin which usually occurs from age 5 through adult life.
We have experienced two cases of EDP in children aged 2 and 3, both exceptionally younger than the previously reported cases. We therefore suggest that EDP should be included in the differential diagnosis of pigmentary disorders occurring at an early age.
=================================================================
15.) Fixed drug eruption presenting as erythema dyschromicum perstans: a flare without taking any medications.
=================================================================
Dermatology 1998;197(4):383-5
Mizukawa Y, Shiohara T
Department of Dermatology, Kyorin University School of Medicine, Tokyo, Japan.
Fixed drug eruption (FDE) can present as multiple pigmented macules that flare at fixed sites even when the patient has taken no medications. Although this presentation is not characteristic of FDE, it must be borne in mind in order to make a correct diagnosis. We describe such a patient whose condition was initially diagnosed as erythema dyschromicum perstans (EDP). Immunohistochemically intraepidermal T cells were distributed between basal and suprabasal keratinocytes in the lesional skin, a finding suggestive of FDE.
A flare occurred not only with exposure to theophylline but also without exposure. A flare has never recurred and pigmented macules faded gradually after avoiding theophylline. On the basis of these findings, we recommend that patients with an EDP-like presentation be examined completely for causes such as drugs before labeling the cutaneous lesions.
=================================================================
16.) Reticulate postinflammatory hyperpigmentation with band-like mucin deposition.
=================================================================
Int J Dermatol 1998 Nov;37(11):829-32
Noto G, Pravata G, Arico M
Department of Dermatology, University of Palermo, Policlinico P. Giaccone, Italy.
BACKGROUND: Mucinoses of the skin are a group of disorders sharing accumulation of mucin in the skin or hair follicles. Postinflammatory hyperpigmentation, with pigmentary incontinence, is due to loss of melanin from epidermal basal cells and its accumulation in dermal macrophages. METHODS: We describe clinicopathologic features of two patients presenting with the association of pigmentary incontinence with an unusual diffuse, band-like dermal deposition of mucin, clinically presenting with reticular pigmented macular lesions.
RESULTS: Two patients were observed with asymptomatic, persistent, reticular, pigmented patches located in the flexures, thighs, neck and back. Histology showed melanophages with a diffuse, band-like dermal deposition of mucin, an increased number of fibroblasts, a slight T-cell infiltrate and scattered mast cells. Blood markers of lupus erythematosus were negative.
CONCLUSIONS: These findings may draw attention to pigmentary disorders such as lichen planus pigmentosus, erythema dyschromicum perstans, pigmentatio maculos eruptiva idiopathica, dermatopathia pigmentosa reticularis, prurigo pigmentosa and frictional melanosis.
None of these entities, however, includes mucin deposition among its microscopic features. Macules were not preceded by erythema or any other lesions. We suggest that our cases could belong to group II of Rongioletti and Rebora's classification, i.e. they could be cases of secondary mucin deposition in postinflammatory hyperpigmentation, possibly in an unusual form of lichen planus pigmentosus or, less likely, frictional melanosis.
=================================================================
17.) Erythema dyschromicum perstans: report of a new case and critical review of the literature.
=================================================================
J Dermatol 1998 Nov;25(11):747-53
Combemale P, Faisant M, Guennoc B, Dupin M, Heyraud JD
Department of Dermatology, Military Hospital Desgenettes, Lyon, France.
Erythema dyschromicum perstans (EDP), described by Convit et al. in 1961, is a rare dermatosis. Its relationship with ashy dermatosis (AD), described by Ramirez in 1957, is still a matter of debate.
We report a typical case of EDP. The patient, of North African origin, had a dyschromic (hypo- and hyperpigmented) eruption on the chest and limbs for 2 years. The lesions were occasionally surrounded by a papular border which spread slowly and centrifugally. Histological examination showed a lichenoid infiltrate. A carcinoma of the lung was simultaneously discovered.
No treatment was given, EDP is infrequent and often considered identical to ashy dermatosis in the literature. However, the clinical aspects of the two diseases differ. The main features of these two diseases are reviewed and compared on the basis of a literature review. We conclude that EDP and AD are distinct clinical entities.
=================================================================
18.) Involvement of cell adhesion and activation molecules in the pathogenesis of erythema dyschromicum perstans (ashy dermatitis). The effect of clofazimine therapy.
=================================================================
Arch Dermatol 1997 Mar;133(3):325-9
Baranda L, Torres-Alvarez B, Cortes-Franco R, Moncada B, Portales-Perez DP, Gonzalez-Amaro R
Department of Immunology, School of Medicine, University of San Luis Potosi, Mexico City, Mexico.
OBJECTIVES: To assess the expression of several cell adhesion and lymphocyte activation molecules in erythema dyschromicum perstans lesions, and to evaluate the effect of clofazimine therapy on the expression of these molecules.
DESIGN AND METHODS: A prospective study. Skin biopsy samples were obtained from patients before and after 3 months of clofazimine therapy, and the expression of cell adhesion and activation molecules was assessed by an immunohistochemical technique.
SETTING: This study was performed in a clinical referral center and an immunology research laboratory.
PATIENTS: We studied 6 patients with erythema dyschromicum perstans. A diagnosis was made on the basis of clinical and histological criteria. Two patients discontinued participation in the study: one because of adverse effects and the other for unknown reasons.
INTERVENTIONS: Patients were treated with clofazimine, 100 mg/d, for 3 months.
MAIN OUTCOME MEASURES: Expression of cell adhesion and lymphocyte activation molecules in skin biopsy specimens before and after clofazimine therapy. RESULTS: Before clofazimine therapy, we detected a noticeable expression of intercellular adhesion molecule 1 and major histocompatibility complex class II molecules (HLA-DR) in the keratinocyte basal cell layer. In addition, CD36, a thrombospondin receptor that is not expressed by normal skin, was detected in the strata spinosum and granulosum. The dermal cell infiltrate expressed the activation molecule AIM/CD69 and the cytotoxic cell marker CD94. After clofazimine therapy, the expression of intercellular adhesion molecule 1 and HLA-DR disappeared, as well as the mononuclear cell infiltrate.
CONCLUSIONS: Our results suggest that some cell adhesion and activation molecules are involved in the pathogenesis of erythema dyschromicum perstans. Clofazimine appears to have an important effect on the inflammatory phenomenon of erythema dyschromicum perstans.
=================================================================
19.) Periorbital hyperpigmentation and erythema dyschromicum perstans.
=================================================================
Can J Ophthalmol 1992 Dec;27(7):353-5
Ing EB, Buncic JR, Weiser BA, de Nanassy J, Boxall L
University of Toronto, ON.
Erythema dyschromicum perstans is a rare idiopathic dermatosis characterized by ash-grey, well-demarcated skin lesions, which may involve the face.
We describe an 8-year-old girl with erythema dyschromicum perstans presenting as bilateral acquired periorbital hyperpigmentation. The changes seen on histologic study of a skin biopsy specimen were consistent with the clinical diagnosis. The various causes of periorbital hyperpigmentation and characteristics of erythema dyschromicum perstans are reviewed.
=================================================================
20.) Erythema dyschromicum perstans and lichen planus: are they related?
=================================================================
J Am Acad Dermatol 1989 Aug;21(2 Pt 2):438-42
Berger RS, Hayes TJ, Dixon SL
Wilford Hall USAF Medical Center, Lackland Air Force Base, Texas.
A 53-year-old woman initially had lichen planus primarily on her extremities. Approximately 1 year later, lesions consistent with erythema dyschromicum perstans were observed. Both diseases cleared with griseofulvin therapy but returned after discontinuation of the drug. Retreatment with griseofulvin again resulted in clearing.
=================================================================
21.) Erythema dyschromicum perstans. Immunopathologic studies.
=================================================================
J Am Acad Dermatol 1989 May;20(5 Pt 2):882-6
Miyagawa S, Komatsu M, Okuchi T, Shirai T, Sakamoto K
Department of Dermatology, Nara Medical University, Japan.
Immunopathologic studies of a patient with clinical and histologic evidence of erythema dyschromicum perstans revealed Ia antigen expression on epidermal keratinocytes, pronounced OKT4 and OKT6 staining of epidermal dendritic cells, and dermal infiltration of T lymphocytes of both helper-inducer (OKT4) and suppressor-cytotoxic (OKT8) phenotypes--a pattern commonly associated with lichen planus. These findings, taken in conjunction with positive IgG staining on colloid bodies, suggest the possibility that erythema dyschromicum perstans and lichen planus have similar disease processes.
=================================================================
22.) Simultaneously active lesions of vitiligo and erythema dyschromicum perstans.
=================================================================
Arch Dermatol 1988 Aug;124(8):1258-60
Henderson CD, Tschen JA, Schaefer DG
Departments of Pathology, Baylor College of Medicine, Houston, Tex.
Recently, a patient presented to us with skin that had areas of normal pigmentation, hyperpigmentation, and depigmentation. Workup eventually showed him to have simultaneously active lesions of a depigmenting disorder, vitiligo, and a hyperpigmenting disorder, erythema dyschromicum perstans.
=================================================================
23.) Mononuclear cell subpopulations and infiltrating lymphocytes in erythema dyschromicum perstans and vitiligo.
=================================================================
Histol Histopathol 1987 Jul;2(3):277-83
Gross A, Tapia FJ, Mosca W, Perez RM, Briceno L, Henriquez JJ, Convit J
Institut of Biomedicine, Caracas, Venezuela.
Erythema dyschromicum perstans (EDP) and vitiligo are two cutaneous pigmentary dermatoses of unknown etiology. In the present study, the leukocyte infiltrates in the affected skin of EDP and vitiligo patients were studied using the avidin-biotin (ABC) immunoperoxidase technique and monoclonal antibodies which recognise the following mononuclear cell subgroups: T-suppressor/cytotoxic (CD8-Leu-2), T-helper (CD4 = OKT4), T-suppressor + macrophages (Leu-15), Pan T (CD3 = Leu-4), macrophages (Leu-M3) and Langerhans cells (CD1 = Leu-6), and other cellular markers such as Ia antigens and the Interleukin-2 receptor (CD25 = TAC).
The immunocytochemical analysis showed a selective accumulation of CD3+, CD8+, Leu-15-, T-cytotoxic cells in the epidermis of both EDP and early lesions of vitiligo.
In addition, an increase in the number of epidermal Langerhans cells (CD1+) was observed in some cases of EDP and vitiligo. The CD4/CD8 ratios in affected and uninvolved skin for both disorders were not significantly different, although values lower than unity were only observed in the infiltrates of affected skin. Ia antigen positivity was observed in the dendritic cells of the dermis and epidermis, as well as in most of the lymphoid cells within the infiltrates for both diseases. Macrophages (Leu-M3) in EDP dermal infiltrates were generally found adjacent to extracellular melanin pigment.
Lymphocytes expressing TAC (CD25) surface antigens were also present in the dermal infiltrates. These morphological observations suggest a possible immune cell participation in the dyschromia of such cutaneous disorders.
=================================================================
24.) Chlorothalonil, a possible cause of erythema dyschromicum perstans ( ashy dermatitis).
=================================================================
Penagos H; Jimenez V; Fallas V; O'Malley M; Maibach HI
Occupational Dermatology Service, Social Security Hospital, Panama.
Contact Dermatitis (DENMARK) Oct 1996 35 (4) p214-8 ISSN: 0105-1873
Language: ENGLISH
Document Type: JOURNAL ARTICLE
Journal Announcement: 9705
Subfile: INDEX MEDICUS
We studied 39 patients with erythema-dyschromicum-perstans-like dermatitis seen at Changuinola Hospital in Panama. They were compared with 41 controls.
The 2 groups were native field workers of the banana plantations exposed to many pesticides. In 34 patients, there was a positive patch test reaction to 2,4,5,6-1,3- tetrachloroisophthalonilnitrile (chlorothalonil, TCPN) 0.001% in acetone. In 39 cases, biopsies showed a lichenoid tissue reaction compatible with a chronic pigmented dermatitis or erythema-dyschromicum-perstans-like dermatitis.
Chlorothalonil is possibly the cause of the pigmented dermatitis observed in the 39 banana farm workers studied. Until additional studies are carried out, we consider this a possible rather than definite cause-and-effect relationship.
=================================================================
25.) Lichen planus pigmentosus presenting in zosteriform pattern.
=================================================================
Cho S; Whang KK
Department of Dermatology, College of Medicine, Ewha Womans University,
Seoul, Korea.
J Dermatol (JAPAN) Mar 1997 24 (3) p193-7 ISSN: 0385-2407
Language: ENGLISH
Document Type: JOURNAL ARTICLE
Journal Announcement: 9709
Subfile: INDEX MEDICUS
Lichen planus pigmentosus (LPP) has thus far been described as a condition of unknown etiology which clinically differs from the classical lichen planus (LP) by exhibiting dark brown macules and/or papules mostly in exposed areas and flexural folds and a longer clinical course without pruritus or scalp, nail or mucosal involvement.
Histopathologically, LPP shows the typical changes seen in LP, but with thinning of epidermis. We report a case of LPP that developed in a unilateral, zosteriform pattern on the left flank of a 49-year-old man.
This case seems to lie in the middle of the spectrum between classical LP and ashy dermatosis, and, to the best of our knowledge, is the first report of LPP presenting in the zosteriform pattern.
=================================================================
26.) [Erythema dyschromicum perstans versus lichen planus].
=================================================================
Med Cutan Ibero Lat Am 1987;15(1):89-92
Leonforte JL, Pelaez de di Bari O
Erythema dyschromicum perstans and lichen planus have been regarded as related. We describe the case of a 41 year old man presenting a relapsing dermatitis consisting of erythematous patches leaving behind ashy-gray macules. The lesions of lichen planus were atypical and the ashy dermatosis was transient. The possibility that some cases of lichen planus lead to an erythema dyschromicum perstans is discussed.
=================================================================
27.) Erythema dyschromicum perstans.
=================================================================
Cutis 1986 Jan;37(1):42-4
Lambert WC, Schwartz RA, Hamilton GB
A 29-year-old woman from Trinidad experienced the rapid onset of extensive lesions characteristic of erythema dyschromicum perstans following an x-ray study using orally administered contrast.
Eleven months later a skin biopsy specimen showed few epidermal changes but extensive incontinence of melanin pigment and marked dilatation of lymphatics in the superficial dermis. Results of a systemic evaluation were normal. The available data on this disease are analyzed and conclusions offered regarding its nature and causes.
=================================================================
28.) Erythema dyschromicum perstans.
=================================================================
J Am Acad Dermatol 1980 Apr;2(4):295-302
Tschen JA, Tschen EA, McGavran MH
Erythema dyschromicum perstans (EDP) was first described in 1957, and electron microscopic studies were reported in 1969. Herein, we describe five cases and compare light and electron microscopic findings, direct and indirect immunofluorescence, and dopa-positive melanocyte counts between normal and affected skin.
The results indicate that EDP is a clinically characteristic disorder with a lichenoid reaction in its active phase. This lichenoid reaction leads to a pronounced incontinence of pigment and to decreased numbers of melanocytes and of tyrosinase activity in the involved epidermis. These findings support the suggestion that EDP and lichen planus pigmentosus are possible the same entity.
Direct inmunofluorescence and fine structural studies show similar findings to lichen plunus. Patients have low-titer antibodies to extranuclear basal cell components.
=================================================================
29.) [Erythema cinitiensis perstans].
=================================================================
Med Cutan Ibero Lat Am 1980;8(1-3):11-4
Sittart JA, Tayah M
The authors report a case of Erythema Cinitiensis Perstans, in a thirty-one years old white man. This dermatosis, reported in the literature also es Ashy Dermatitis and Erythema Dyschromicum Perstans, is here in Brazil exceptional. Clinically this dermatosis is characterized by the presence of gray patches in a sometimes surrounded by an erythematous active border. The lesions may occur on any area of the integument, sparing the hair scalp, palms, soles and nails.
The therapy has been ineffective in all the cases, but one reported by Stevenson and Miura and in our case, where the patients have improved after Dithiazanine iodide treatment due to intestinal parasitoses by the Tricocephalus trichiurus.
=================================================================
30.) [Idiopathic eruptive macular pigmentation].
=================================================================
Ann Dermatol Venereol 1978 Feb;105(2):177-82 PORTUGAL
Degos R, Civatte J, Belaich S
The feeling of the authors is that their seven reported cases of a pigmented dermatosis are different from the ashy dermatosis and from the erythema dyschromicum perstans.
This disease, which affects children and teenagers, males as well as females, is characterized by pigmented macules 5-25 mm in diameter, affecting the neck, the trunk and the limbs. The first symptom is whether a pigmented spot, or an erythematous, papular or achromic lesion; in the latter instance the pigmentation occurs only secundarily. In most of the cases this dermatose is slowly and spontaneously regressive.
The histological picture is not really specific. In one case there was a marked intraepidermal dyskeratosis of the sweat duct openings. The etiology remains unknown.
=================================================================
31.) [Erythema dyschromicum perstans].
=================================================================
Hautarzt 1977 Oct;28(10):539-41
Moller-Vietheer M, Goos M
The case of a 4 1/2 year old girl with the typical clinical picture of erythema dyschromicum perstans is presented. A survey of the literature on this dermatosis is described.
=================================================================
32.) Erythema dyschromicum perstans. A follow-up study from northern Finand.
=================================================================
Dermatologica 1977;155(1):40-4
Palatsi R
Four patients with ashy dermatosis are described. Their ages varied from 8 to 12 years. Three had typical widespread macular eruptions and one had a linear lesion not described before. The follow-up investigation revealed that the eruption disappeared within 2 years in three of the patients. One patient could not be followed. The duration of the disease and the linearity of one lesion resembled lichen ruber planus.
=================================================================
33.) Ingestion of ammonium nitrate as a possible cause of erythema dyschromicum perstans (ashy dermatosis).
=================================================================
Dermatologica 1975;150(5):287-91
Jablonska S
Clinically and histologically typical erythema dyschromicum perstans has been provoked by repeated ingestion of very small amounts of a fertilizer, ammonium nitrate.
It has been used by a boy who has noticed accidentally that after licking the fertilizer he developed hyperpigmentations. His main purpose was to avoid school attendance, and he developed a very ingenious method of licking the fertilizer once in several weeks in such a way that it did not produce any digestive or other troubles.
His brother, an uniovular twin who had no contact with ammonium nitrate, was healthy. The case supports Pinkus' hypothesis that this type of lesions may be related to some environmental contaminant. Attention is called to a possible food contamination by ammonium nitrate.
=================================================================
34.) [Erythema dischromicum perstans (ashy dermatosis). Report of two cases]. Pathologica 1993 Sep-Oct;85(1099):533-41
=================================================================
[Article in Italian]
Paradisi M, Mostaccioli S, Celano G, Angelo C, Ruatti P, Ferranti G, Onetti
Muda A, Faraggiana T
IV Divisione e Dermatologia Pediatrica, IDI-IRCCS, Roma.
Clinical, histological and ultrastructural investigations of two cases of Erythema Dischromicum Perstans (EDP) are reported. EDP is a chronic pigmented lesion of the skin, and its etiology is still unknown. The reported cases showed clinical and ultrastructural differences from what already described in the literature.
EDP is also difficult to differentiate from other cutaneous pigmented lesions: clinical and morphologic differences and/or similarities are therefore discussed and compared. The usefulness for a correct diagnosis of the co-existence of optical and ultrastructural lesions which are not pathognomonic per se, is also stressed.
=================================================================
35.) [Ashy dermatosis].
=================================================================
Vestn Dermatol Venerol 1989;(11):57-8
[Article in Russian]
Kasimov N, Kiiamov FA, Naimova MR
Five patients with ashy dermatitis are described, aged 6 to 14, one boy and four girls. The process is characterized by dirty grayish or ash-gray-colored maculae on the skin of the trunk and limbs.
These maculae do not tend to fuse, nor exfoliate; they are not associated with any subjective sensations. Thorough examinations have not revealed any osteomuscular or visceral abnormalities.
The disease runs a benign course, and only the cosmetic defect worries the patients.
=================================================================
36.) [Ashy dermatosis. Review of the literature and report of a case].
=================================================================
Med Cutan Ibero Lat Am 1988;16(1):31-6
[Article in Portugese]
de Azevedo LM, Porto JA
Servico de Dermatologia do Hospital Universitario Pedro Ernesto, da Universidade do Estado do Rio de Janeiro.
The authors make a review of the epidemiologic, etiopathogenic, clinical, laboratory and therapeutic aspects of ashy dermatosis, described in 1957 by Ramirez in El Salvador, of which more than 150 cases have been described up to now in different continents. The disease is exclusively cutaneous, presents peculiar clinical features with a lichenoid tissue reaction, and has no specific treatment or known etiology.
The authors report a case in a Brasilian man, followed up for three years. The treatment of a T. trichiura infestation did not change the cutaneous features, as opposed to what has been reported.
=================================================================
37.) [Ashy dermatosis (erithema dyschromicum perstans): prospective study of 23 patients].
=================================================================
Med Cutan Ibero Lat Am 1988;16(5):407-12
[Article in Spanish]
Navarro Jimenez BR, Sanchez Navarro LM
Servicio de Dermatologia, Universidad Autonoma, Benito Juarez, Oaxaca, Mexico.
During the period between january 1984 to july 1987 in the Hospital Unit "Presidente Juarez" ISSSTE, Oaxaca (Mexico), for the first time was given dermatology consult to 2,683 patients among them, 23 who had ashy dermatosis (Erithema dyschromicum perstans), a study was done for the present time and the future of the same, discarding it as possible cause of that nosological entity: treponemal disease, parasitic, infectious, hepatic and renal.
It is commented in relation with the ashy dermatosis and lichen planus, the clinicals variants and the possible sun etiology.
=================================================================
38.) Reticulate, patchy and mottled pigmentation of the neck. Acquired forms.
=================================================================
Dermatology 1998;197(3):291-6
Lautenschlager S, Itin PH
Outpatient Clinic of Dermatology, Triemli Hospital, Zurich, Switzerland.
Besides the inherited forms of mottled and reticulate pigmentation, a vast number of diseases and trigger mechanisms can lead to acquired pigmentation of the neck. Nonhereditary variants of reticulate and mottled pigmentation can affect the neck as a typical site and therefore may give a diagnostic clue or it can occur sporadically on the neck as well as on other sites. A well-known and important factor in the pathogenesis is exposure to sunlight.
Sun-induced pigmentation often presents on the neck and may result from phototoxic, photoallergic and cumulative actinic damage. Frequent forms comprise berloque dermatitis, Riehl's melanosis, poikiloderma of Civatte and tanning bed lentigines. Different infections may also lead to this distinct skin alteration as pediculosis capitis, pityriasis versicolor and syphilis II.
Treatment-induced irregular pigmentations may occur after applications of topical agents (e.g. diphenylcyclopropenone), systemic medication (e.g. 5-fluorouracil, chlorpromazine), as a complication of laser resurfacing or as a chronic graft-versus-host reaction. Different neoplasms may also involve the neck. Widespread pigmented basal cell carcinoma, cutaneous T-cell lymphoma, syringolymphoid hyperplasia and histiocytic diseases may lead to reticulated pigmentation.
Various other infrequent conditions as connective tissue diseases, malnutrition, lichen planus pigmentosus and others are summarized. The neck, a readily accessible site to medical inspection, may have an underestimated value for the diagnosis of different skin diseases.
=================================================================
39.) Lichen planus pigmentosus associated with acrokeratosis of Bazex.
=================================================================
Clin Exp Dermatol 1994 Jan;19(1):70-3
Sassolas B, Zagnoli A, Leroy JP, Guillet G
Department of Dermatology, C.H.U. Brest, France.
A patient with an acquired pigmentation related to lichen planus pigmentosus is described. Features of acrokeratosis of Bazex were associated, related to a head and neck carcinoma. Both cutaneous conditions disappeared after treatment of the neoplasia. Diagnostic criteria of lichen planus pigmentosus are reviewed. The paraneoplastic nature of this original observation of lichen planus pigmentosus is discussed.
=================================================================
40.) Ashy dermatosis and lichen planus pigmentosus: a clinicopathologic study of 31 cases.
=================================================================
Int J Dermatol 1992 Feb;31(2):90-4
Vega ME, Waxtein L, Arenas R, Hojyo T, Dominguez-Soto L
Department of Dermatology, Hospital General Dr. Manuel Gea Gonzalez, Mexico City, Mexico.
The clinical and histopathologic characteristics of patients with ashy dermatosis (n = 20) and lichen planus pigmentosus (n = 11) were analyzed. We found significant clinical differences between both dermatoses, supporting our opinion that they are two separate conditions. Both dermatoses were histologically similar.
=================================================================
41.) [Lichen ruber exanthematicus et pigmentosus in mercury poisoning. A contribution to individual pathology in occupational medicine].
=================================================================
Z Hautkr 1990 Nov;65(11):1013-8, 1021
[Article in German]
Marsch WC, Groebe G
Zentrum der Dermatologie und Venerologie, Abteilung I, Johann Wolfgang Goethe-Universitat, Frankfurt am Main.
We report on a 21-year-old man professionally exposed to mercury, who developed lichen planus. This case must be regarded as a dispositional reaction and is in Germany entitled to indemnification in terms of a "quasi-occupational disease".
The clinical signs and the probably non-allergic pathomechanism are comparable with those of lichen planus induced by gold. In diseases due to occupational intoxication, we face an individual disposition regarding the degree of clinical symptoms, which has to underly any expert opinion on indemnity.
=================================================================
42.) [Lichen planus and lichen planus pigmentosus following gold therapy--case reports and review of the literature].
=================================================================
Z Hautkr 1986 Mar 1;61(5):315-9
[Article in German]
Ingber A, Weissmann-Katzenelson V, David M, Bialowons M, Feuerman EJ We report on two typical cases of lichen planus and lichen pigmentosus appearing after gold therapy. The characteristics of lichen planus induced by drugs are emphasized, and the literature is reviewed.
=================================================================
43.) Lichen planus pigmentosus of the oral mucosa: a rare clinical variety.
=================================================================
Dermatologica 1981;162(1):61-3
Laskaris GC, Papavasiliou SS, Bovopoulou OD, Nicolis GD
In this paper, we describe a case of lichen planus of the mouth with intense melanosis, in a middle-aged white male. Due to its unusual clinical characteristics, we believe that this case represents a rare variant of lichen planus of the oral mucosa. The histopathologic findings, differential diagnosis and its possible connection with lichen planus pigmentosus of the skin are discussed.
===================================================================
DATA-MÉDICOS/DERMAGIC-EXPRESS No (73) 29/09/99 DR. JOSÉ LAPENTA R.
UPDATED 14 JUNE 2025
===================================================================
Produced by Dr. José Lapenta R. Dermatologist
Venezuela 1.998-2.025
Producido por Dr. José Lapenta R. Dermatólogo Venezuela 1.998-2.025
Tlf: 0414-2976087 - 04127766810


















.png)